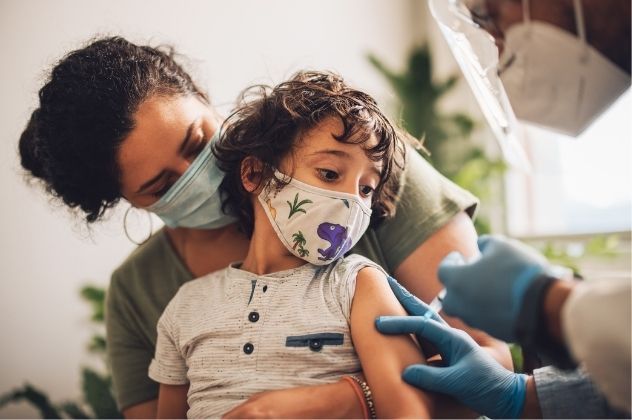
But what can parents do to help prepare their child for the COVID-19 Pfizer vaccine or other injections?
NEEDLE PHOBIA
Most children are fearful of needles. But for some children, this fear is more serious and can be defined as a needle phobia.
Needle phobia is a very scary and distressing response to the presence of or reaction to a needle, for example, to take blood or have an injection. The anxiety and fear are out of proportion to the threat, and people will avoid needles as much as possible.
In severe cases, the level of anxiety caused by just the sight of a needle may result in feelings of dizziness, nausea, increased sweatiness, loss of consciousness, and fainting.
Almost one in five children (19%) aged 4-6 have a needle phobia, and this decreases to one in nine (11%) by age 10-11. Among adults, about 3.5-10% have a needle phobia.
Working as a nurse, I still remember Emma, a five-year old girl, who was petrified of needles. I recall her little face, the anger and fear, the tears and screams just at the sight of a needle.
Her increasing fear was due to previous blood tests, injections, and other medical procedures. And it didn’t get any easier until she got some professional play therapy help.
When booking vaccination appointments, consider asking the nurse to set aside extra time to prepare.
When children come for a vaccination, most nurses anticipate the child may be concerned and nervous, or very frightened of an injection.
Nurses may help by asking the child to tense and relax their muscles to prevent fainting. They may suggest taking a deep breath, holding it and breathing out slowly. They may also ask the child to wiggle their toes to provide some distraction.
If the child is obviously distressed – for example, screaming, kicking and saying they don’t want it – parents can postpone the needle so the child has an opportunity to develop some coping strategies. This could potentially prevent a needle phobia from developing.
COPING STRATEGIES
Parents are the best advocates for their child and know how to support them during their immunisations.
The first step is to consider when to give your child information about the vaccine. For children under five years, a shorter time frame works better; for example, the same day.
For children five to six years, you might tell them up a day or two before; and for those seven years, up to a week before.
But if your child has a needle phobia, they may need significant help in a safe environment to play out their thoughts and feelings, and learn some stress management strategies.
Qualified play therapists, child life therapists and child psychologists can help. After building a trusting relationship with the therapist, medical play therapy sessions involve role-playing scenarios to desensitise the child to medical equipment.
This often starts with toy medical equipment and moves towards more authentic medical equipment.
The therapist provides information to the child by showing them how things work. The child may then develop mastery by injecting their doll or teddy, while the therapist provides cues for coping strategies and resiliency.
Some children need one or two sessions, but those with a needle phobia may require up to ten sessions or more.
Therapists can also teach parents skills to support their child during a needle or other medical procedure.
Introduce some pretend medical equipment toys to your child’s playtime and notice if they’re curious or avoid them.
If they’re curious and seek more information, show and tell them about their upcoming vaccine and why they need it. You might say, for instance, it will help to stop them, and lots of other people, from getting the coronavirus, including their grandparents.
Children are aware from media and school that COVID has forced people to stay at home because it made many people sick, and they couldn’t breathe properly. You might explain that protection from the vaccine will help them stay at kinder or school and see their friends.
For the child who avoids playing with the medical toys, distraction techniques may help. Consider introducing a new toy or object that can hold the child’s attention immediately before and during the injection. This might be sensory fidget toys, I-spy books, digital games or apps.
For Emma, after developing a therapeutic play relationship, I introduced and practised the Magic Glove Technique. For children with good imaginations, they can learn to relax and pretend they have a magic invisible glove that makes their arm – and themselves – feel calm and relaxed.
For other children, I have used Buzzy, a mechanical vibrating device that looks like a bee, developed by American physician and pain researcher Amy Baxter. It has a cold pack and the vibration inhibits the sensation of pain.
If your child has a negative experience during their vaccination, and you’d like to access professional help, ask your GP for suggestions of local play therapists or child life therapists or child psychologists in your area.